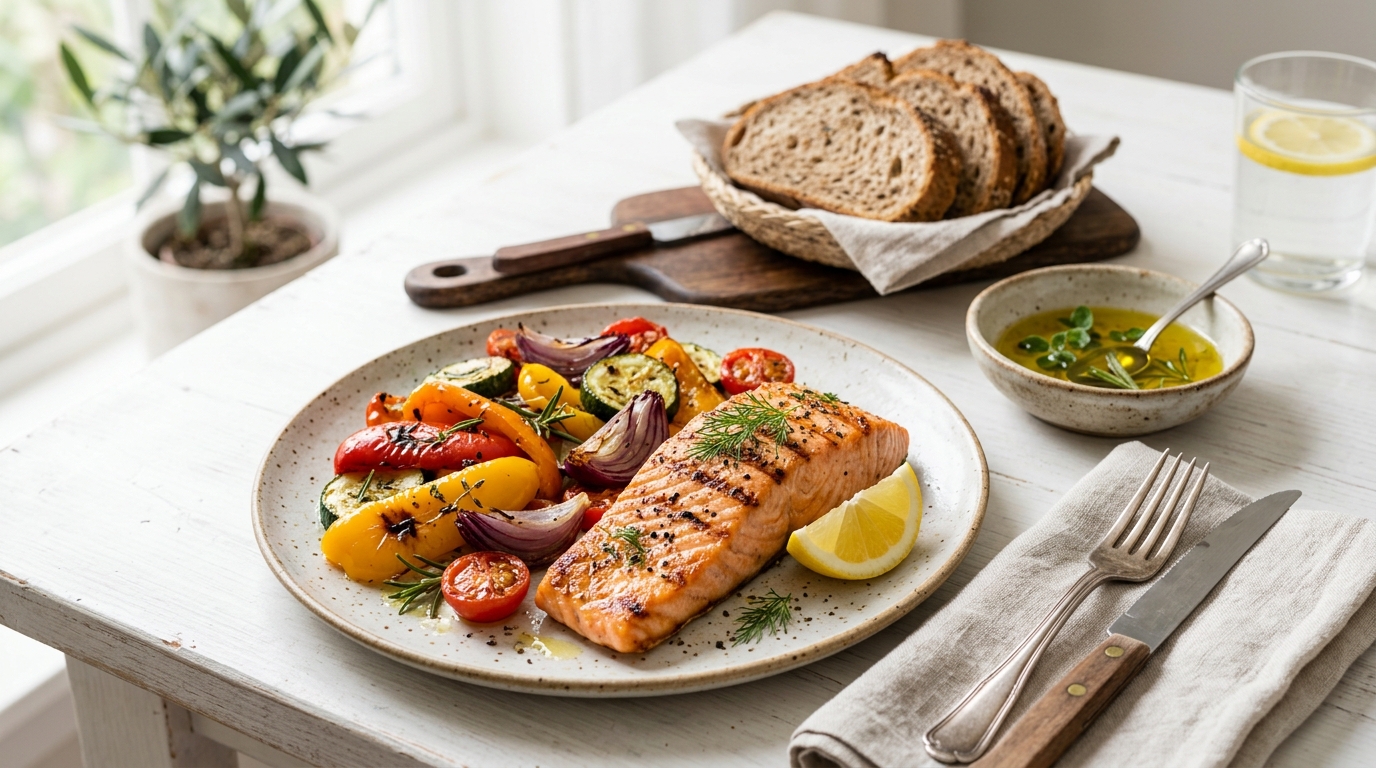Introduction
The relationship between diet and heart health is one of the most thoroughly studied areas in all of nutritional medicine. Decades of research — from population studies to controlled clinical trials — have established that what we eat profoundly influences virtually every measurable cardiovascular risk factor: cholesterol levels, blood pressure, systemic inflammation, blood sugar stability, arterial elasticity, and body weight. Understanding how these mechanisms work helps clarify why certain dietary patterns are so consistently associated with either cardiovascular protection or elevated risk.
This guide walks through the science of how diet affects the heart, which dietary patterns have the strongest evidence base, and what practical changes have the most meaningful impact on long-term cardiovascular health.
Why Diet Is Central to Cardiovascular Health
The heart and vascular system are constantly remodeling in response to the chemical environment created by the foods we eat. Fats influence cholesterol transport and arterial wall composition. Carbohydrates affect blood sugar, triglycerides, and insulin sensitivity. Sodium influences blood volume and pressure. Antioxidants and polyphenols determine how effectively the body counters oxidative damage to blood vessel walls.
Unlike genetics — which cannot be changed — diet is one of the most modifiable cardiovascular risk factors available. Studies suggest that dietary choices account for a substantial proportion of heart disease cases, with estimates from the Global Burden of Disease study indicating that poor diet contributes to more cardiovascular deaths globally than any other single risk factor.
How Diet Affects Your Heart Health
1. Dietary Fat and Cholesterol Metabolism
Not all fats affect the heart the same way. Saturated fats, found primarily in red meat, butter, and full-fat dairy, raise LDL cholesterol by reducing the number of LDL receptors on liver cells, allowing more LDL to circulate in the bloodstream. Trans fats are even more harmful — they raise LDL and simultaneously lower HDL. Monounsaturated fats, found in olive oil and avocados, improve cholesterol ratios. Omega-3 fatty acids reduce triglycerides and arterial inflammation. Choosing predominantly unsaturated fats while minimizing saturated and trans fats is one of the most evidence-backed dietary interventions for heart health.
2. Dietary Fiber and Arterial Health
Soluble fiber binds bile acids in the digestive tract, reducing their reabsorption and forcing the liver to draw on circulating cholesterol to produce more. This mechanism directly lowers LDL levels. Insoluble fiber, meanwhile, supports gut microbiome diversity, reduces systemic inflammation, and improves insulin sensitivity — all of which have cardiovascular downstream effects. Most adults consume far less fiber than the recommended 25 to 38 grams per day, and increasing intake from whole grains, legumes, fruits, and vegetables is associated with significantly lower rates of heart disease.
3. Sodium, Potassium, and Blood Pressure
Blood pressure is heavily influenced by the ratio of sodium to potassium in the diet. Sodium increases blood volume and stimulates arterial constriction, while potassium counteracts both effects and promotes sodium excretion through the kidneys. The typical Western diet is characterized by excess sodium and inadequate potassium — the precise imbalance most associated with hypertension. Shifting toward a diet with less processed food and more whole plant foods naturally corrects this ratio.
4. Sugar, Refined Carbohydrates, and Triglycerides
High intake of added sugars and refined carbohydrates raises blood triglycerides — lipids that are independently associated with cardiovascular risk. It also promotes insulin resistance, which impairs the liver’s ability to process lipids normally and leads to higher circulating LDL and lower HDL. The fructose component of added sugar is metabolized primarily in the liver, where excess amounts are converted to fat, contributing to fatty liver disease and metabolic syndrome — both of which compound cardiovascular risk.
5. Antioxidants and Vascular Inflammation
Oxidative stress damages the endothelium — the thin layer of cells lining blood vessels — and promotes the oxidation of LDL cholesterol, which is the form that most readily accumulates in arterial plaques. Foods rich in antioxidants, particularly vitamins C and E, polyphenols, and carotenoids, reduce oxidative damage to vascular tissue. Berries, green tea, dark chocolate, olive oil, and colorful vegetables are among the richest dietary sources.
For a detailed overview of the most nutrient-dense foods to build a heart-supportive diet around, our guide on 10 best healthy foods to eat every day provides a practical starting framework.

6. The Mediterranean Diet and Cardiovascular Outcomes
The Mediterranean diet — characterized by high olive oil consumption, abundant vegetables and legumes, regular fish intake, moderate nuts and fruits, and minimal processed food — has the strongest evidence base of any dietary pattern for cardiovascular protection. The landmark PREDIMED trial found that adherence to the Mediterranean diet reduced major cardiovascular events by approximately 30% compared to a low-fat control diet. It improves nearly every measurable cardiovascular risk factor simultaneously.
7. The DASH Diet and Blood Pressure
The Dietary Approaches to Stop Hypertension (DASH) diet was specifically designed and clinically tested for blood pressure management. It emphasizes fruits, vegetables, whole grains, low-fat dairy, and lean protein while limiting sodium, saturated fat, and added sugar. Clinical trials consistently show that the DASH diet can reduce systolic blood pressure by eight to fourteen points — comparable to many pharmacological interventions for mild to moderate hypertension.
8. Ultra-Processed Foods and Cardiovascular Risk
Ultra-processed foods — defined as industrially formulated products containing additives, preservatives, flavor enhancers, and minimal whole ingredients — are increasingly linked to elevated cardiovascular risk independent of their macronutrient content. Large prospective studies have found that each ten percent increase in ultra-processed food consumption is associated with a twelve percent higher risk of cardiovascular disease. Replacing even a portion of these foods with whole food alternatives meaningfully reduces risk.
9. Dietary Patterns Versus Individual Foods
While individual foods matter, the strongest cardiovascular protection comes from overall dietary patterns rather than any single food or nutrient. A diet that combines fiber from whole grains and legumes, healthy fats from fish and olive oil, antioxidants from fruits and vegetables, and minimal processed food addresses cardiovascular risk at every biological level simultaneously. This is why dietary pattern research consistently outperforms single-nutrient intervention studies in demonstrating cardiovascular benefit.
10. Consistency Over Time
The most important principle in dietary cardiovascular protection is consistency over time. Brief dietary interventions produce temporary changes; sustained eating habits over years and decades accumulate protective effects that become measurable as lower cholesterol, better arterial elasticity, more stable blood pressure, and ultimately lower rates of clinical heart disease. Building a diet that is sustainable and enjoyable — rather than restrictively perfect — is the key to long-term cardiovascular benefit.

Conclusion
The evidence linking diet to heart health is among the most robust in all of medicine. What you eat influences your cholesterol levels, blood pressure, vascular inflammation, triglycerides, insulin sensitivity, and body weight — all of which are direct drivers of cardiovascular disease risk. The dietary patterns with the best cardiovascular evidence — Mediterranean and DASH — share a common theme: whole, minimally processed foods rich in fiber, healthy fats, and antioxidants. Understanding how diet affects your heart provides the foundation for making informed, sustainable choices that protect your cardiovascular health for life.
Frequently Asked Questions
What is the most heart-damaging dietary habit? High consumption of ultra-processed foods — which are simultaneously high in trans fats, saturated fats, sodium, added sugar, and refined carbohydrates — is consistently associated with the greatest cardiovascular harm. This dietary pattern addresses multiple cardiovascular risk factors negatively at once, making it more damaging than any single harmful food consumed in moderation.
Does eating fat cause heart disease? The type of fat matters far more than total fat intake. Saturated and trans fats are linked to elevated LDL cholesterol and cardiovascular risk. Unsaturated fats from olive oil, avocados, nuts, and fish are associated with better cardiovascular outcomes. The outdated idea that all dietary fat is harmful for the heart has been largely revised by modern nutrition science.
How quickly does diet affect heart health markers? Blood pressure and triglycerides can show measurable improvement within two to four weeks of significant dietary change. LDL cholesterol typically shows meaningful reduction within six to twelve weeks. Arterial function and inflammatory markers improve over months of sustained healthy eating. Long-term cardiovascular event risk changes over years of consistent dietary behavior.
Related Articles
10 Best Foods for Heart Health Foods to Avoid for a Healthy Heart How to Start a Healthy Diet for Beginners